In my virtual primary care practice, I often see patients who come in with a variety of complaints—insomnia, chronic headaches, digestive issues, or just a general sense of being “unwell.” While we always investigate physical causes, more often than not, the trail leads back to a silent, pervasive orchestrator: stress.
Understanding stress isn’t just about “relaxing more.” It’s about understanding the biological machinery of your body and learning how to operate the controls.
What exactly is stress?
At its core, stress is a survival mechanism. It’s the body’s reaction to any change that requires an adjustment or response. When you perceive a threat—whether it’s a car swerving into your lane or an aggressive email from your boss—your body initiates the “fight-or-flight” response.
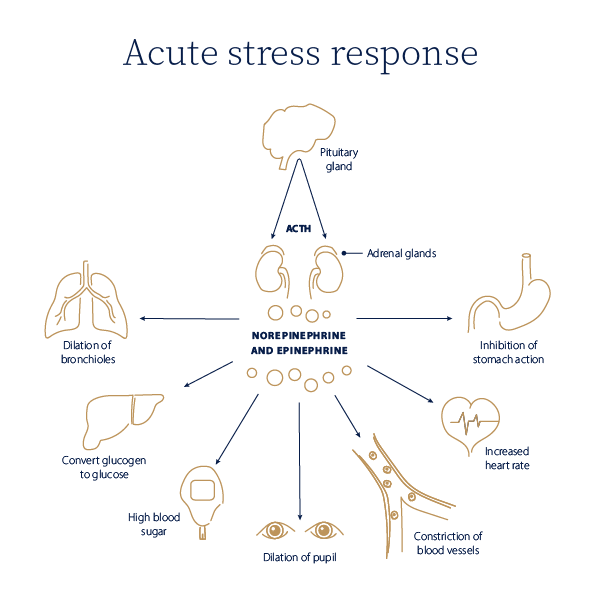
This process starts in the brain’s hypothalamus, which signals your adrenal glands to release a surge of hormones, primarily adrenaline and cortisol.
- Adrenaline: Increases your heart rate, elevates your blood pressure, and boosts energy supplies.
- Cortisol: The primary stress hormone, which increases sugars (glucose) in the bloodstream and enhances your brain’s use of glucose.
This system is magnificent for protection. However, the modern world triggers this high-intensity response for non-life-threatening situations, and many of us never “turn it off.”
How stress manifests: The body’s alarm system
Stress doesn’t just stay in your head; it speaks through your body. Because the stress response affects almost every biological system, the symptoms are incredibly diverse:
- Physical: Tension headaches, muscle pain (especially in the neck and shoulders), chest pain, rapid heartbeat, and frequent colds due to a suppressed immune system.
- Emotional: Irritability, anxiety, feeling overwhelmed, or a lack of motivation.
- Cognitive: Racing thoughts, constant worrying, “brain fog,” and poor judgment.
- Behavioral: Changes in appetite (eating too much or too little), procrastinating, or using negative coping mechanisms.
The domino effect: What chronic stress leads to
When the “fight-or-flight” system stays activated for days or months, it leads to chronic stress, which is a primary underlying driver for several serious health conditions:
- Cardiovascular disease: Constant high blood pressure and heart rate can damage arteries.
- Metabolic issues: Cortisol increases cravings for “comfort foods,” leading to weight gain and potentially Type 2 diabetes.
- Gastrointestinal disorders: Stress can exacerbate GERD (acid reflux), IBS, and stomach ulcers.
- Mental health disorders: Long-term exposure to stress hormones is a major risk factor for clinical depression and anxiety disorders.
Managing the storm: Daily habits and routines
To manage stress, we must focus on down-regulating the nervous system. Think of it as bleeding off the pressure from a steam engine.
1. The power of “micro-rest”
You don’t need a week in the tropics to reset. Implementing “micro-rests” throughout the day can prevent stress from compounding.
- The 90-Minute Rule: Our brains work in ultradian rhythms. Every 90 minutes, take 5 minutes to step away from your screen, stretch, or simply stare out a window.
2. Nutritional resilience
Stress depletes B vitamins and magnesium. Focus on a “stress-busting” diet:
- Complex carbohydrates: Oatmeal and whole grains prompt the brain to produce serotonin.
- Fatty fish: Omega-3s can prevent surges in stress hormones.
- Hydration: Even mild dehydration increases cortisol levels.
3. Sleep hygiene
Sleep is when your brain “cleans” itself of metabolic waste. High cortisol makes it hard to fall asleep, and lack of sleep raises cortisol—it’s a vicious cycle. Aim for a “cool, dark, and tech-free” bedroom.
Inventive ways to cope and prevent
Beyond the standard advice, I encourage my patients to try “system interrupts”:
- The “temperature reset”: If you feel a panic spike, splash ice-cold water on your face or hold an ice cube. This triggers the mammalian dive reflex, which naturally slows the heart rate.
- Box breathing: Breathe in for 4 seconds, hold for 4, exhale for 4, and hold for 4. This is a manual override for your autonomic nervous system.
- Cognitive reframing: Instead of saying “I am stressed,” try saying “I am experiencing a high-energy state.” Reframing the physiological arousal as “readiness” rather than “fear” can change how your body processes the hormones.
When to reach out to your doctor
Self-management is vital, but it has its limits. You should schedule an appointment with your primary care physician if:
- Stress is interfering with your ability to work or maintain relationships.
- You are experiencing physical symptoms like chest pain or chronic digestive issues.
- You feel a sense of hopelessness or are using negative behaviors to cope.
How we can help
A doctor is your partner in your journey to well-being. When you come to us for stress, we don’t just “hand out pills.” We provide:
- Diagnostic screening: To ensure your symptoms aren’t caused by something else, like a thyroid imbalance or vitamin deficiency.
- Referrals: We can connect you with specialized therapists or nutritional counselors.
- Pharmacotherapy: If lifestyle changes aren’t enough, we can discuss short-term or long-term medications to help balance your brain chemistry while you work on other management strategies.
- Actionable monitoring: We can track your blood pressure and markers of inflammation to see how your stress management is physically improving your health.
Stress is an inevitable part of being alive, but it does not have to be the pilot of your life. By understanding that stress is a physical process, you can use physical and mental tools to manage it. You are not “weak” for feeling stressed; you are simply human, reacting to a high-pressure world. Start small. Choose one habit—perhaps just five minutes of breathing or a consistent bedtime—and build from there. If you’re ready to take the first step, schedule an appointment with your HealthTap primary care physician for an evaluation. Virtual visits are included as part of CHM membership! Start today by clicking here, or visit www.healthtap.com/for/chm/.
Editor’s note: It’s important to note that any associated lab, testing, or treatment costs with HealthTap are not included, however, eligible bills can be submitted to CHM for sharing per your program as outlined in the CHM Guidelines. Please refer to the CHM Guidelines and applicable web pages for the most up-to-date information regarding sharing eligibility, CHM membership, and ministry news.



